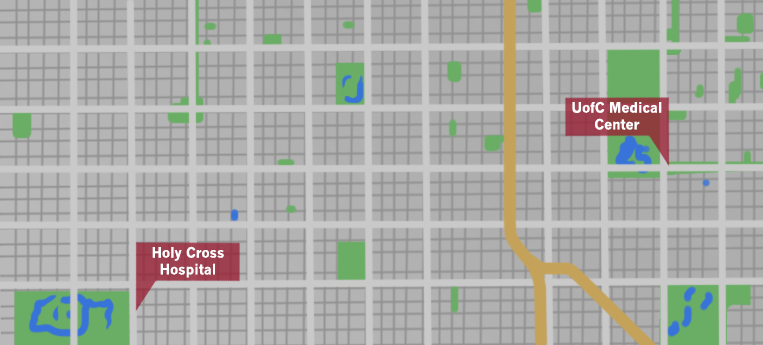
The construction of an Adult Level I Trauma Center on the South Side, long a rallying point for local health equity activism, will likely be realized in the next few years at Holy Cross Hospital in Chicago Lawn. In September, the University of Chicago Medical Center (UCMC) and Sinai Health System, the private, nonprofit hospital group of which Holy Cross is a member, announced a proposal to build a trauma center at the hospital, which administrators of both organizations estimate will take at least two years.
Significantly less certain is how the trauma center will be financed once it is constructed, and the timeline for the bureaucratic checkpoints that are required to bring the facility to fruition. And for the South Side activists who vocally applied public pressure to the UofC, the outcome—a trauma center some distance from Hyde Park—has left some with mixed feelings.
Dr. Gary Merlotti, Chair of Sinai Health System’s Department of Surgery, said that all regional trauma center directors will vote on the proposal at a Region XI EMS meeting on December 17. Region XI EMS is a professional association of all emergency care-providing hospitals in Chicago, and it includes not only nonprofit private institutions like Sinai and UCMC, but also the John H. Stroger, Jr. Hospital of Cook County, which is public. Pending an affirmative vote, the proposal will travel to the Illinois Department of Public Health (IDPH) for state approval.
Last month, the UCMC announced in a statement that it would contribute capital to the project in order to “fund the facility improvements at Holy Cross Hospital, which are estimated to be in the range of $40 million,” and would also staff the trauma center with trauma-related subspecialists in its employ, including “general trauma, neurological, orthopedic and plastic surgeons, urologists, and other areas.” Merlotti said that the UCMC’s contribution of personnel will be critical for the facility to function and noted previous instances of the two organizations sharing human resources.
“We would expect that the majority of people at Holy Cross would be Sinai Health System people, but the UofC is going to be helping us with some of the higher-end people, if you will. In terms of the partnership, it is certainly not written in stone, but it is not a plan that they’re going to dump $40 million to build this building, and just walk away from this. We have had a long-term collaboration with the University of Chicago in many areas. Their residents rotate to our hospital at [Mount] Sinai for Trauma Education, believe it or not,” Merlotti said, in reference to the scale of UCMC’s human resources and budget.
“They are also obviously going to be involved in caring for patients at Holy Cross,” Merlotti added. “The $40 million number is not contractually agreed upon, and the cost of building the trauma center could be higher.”
But he declined to comment on what, exactly, the UofC’s money will be spent on, how the UCMC and Sinai will share the costs of running the trauma center once it is constructed, or what would happen if the facility loses money.
The UCMC is familiar with the last scenario; it occurred when it built an Adult Level I Trauma Center at its main location in Hyde Park in 1986. According to WBEZ, the facility lost $2 million per year until the UofC closed it in 1988. Currently, the UCMC operates a pediatric trauma center that admits patients as old as fifteen years of age. For Merlotti, a critical difference in the financial viability of a trauma center at the present time is that patients who were previously uninsured are covered by the Affordable Care Act.
“The financial milieu for trauma at the present time is somewhat improved because of the Affordable Care Act, and the fact that the majority of people who in the past came to trauma centers in the state uninsured, now they almost always qualify for Medicaid managed care, and we can recoup some of the cost of providing care for them,” Merlotti said. “But this is not going to be a moneymaker, and this is not why we’re going into trying to make this into a trauma center. We’re trying to provide a service to a community around us that needs that service desperately.”
That need, he said, is for high-quality adult trauma care at a hospital that people who live near Chicago Lawn tend to go to because of the inaccessibility of closer facilities, even if they have serious injuries that could warrant transport to an existing trauma center.
However, Merlotti contests the suggestion that physical proximity to a trauma center is critical to preventing South Side trauma deaths.
In 2013, Dr. Marie Crandall, an associate professor of Surgery and Preventative Medicine at Northwestern, and collaborators published “Trauma Deserts: Distance From a Trauma Center, Transport Times, and Mortality From Gunshot Wounds in Chicago” in the American Journal of Public Health, which argued that the absence of a trauma center within five miles of most South Side residents contributed to longer ambulatory transport times for trauma patients, and therefore a higher likelihood of trauma death after transport, than for their North Side counterparts.
“In all honesty, we’re still waiting to collect some data to provide a clear of analysis of this,” Merlotti said. He pointed out that “in the language of Crandall’s research, when this facility is constructed, the most at-risk patients that she identified in her study will be within five miles’ radius at Holy Cross.” He noted, however, that “Dr. Crandall’s ‘Trauma Deserts’ is also not a universally accepted document in the trauma care community; the study has never been replicated. In this type of care, mileage [in transport] is not the critical factor. If you had a supersonic train to get there, you’d be doing well. Time is the issue. Time on the scene, time on the ambulance, time that the hospital takes to intervene.”
Merlotti’s emphasis on time to treatment is consistent with the “Golden Hour” theory, which asserts that a trauma victim’s survival odds decrease substantially after one hour has passed from the time of the incident. However, this viewpoint, like Crandall’s, is not academic consensus. One 2010 study of 3,656 trauma patients, titled “Emergency Medical Services Intervals and Survival in Trauma: Assessment of the ‘Golden Hour’ in a North American Prospective Cohort,” with first author Dr. Craig Newgard of Oregon Health & Science University, found “no significant association” between total time to treatment and mortality.
According to Merlotti, Region XI EMS will consider various studies on the effect of transport times on trauma patient death rates when it meets on December 17 in closed session to discuss and vote on the joint UCMC/Sinai proposal for the trauma center at Holy Cross. He added that the group will also assess the possibility that the plan could draw patients away from the trauma center at Advocate Christ Medical Center in Oak Lawn, although he believes that this is unlikely. If the proposal passes, it will then go to the Illinois Department of Public Health (IDPH) for official approval, after which construction may begin. Sinai and UCMC are not required by law to submit their proposal to the IDPH by any particular date.
Courtney Avery, the administrator for the Illinois Health Facilities and Services Review Board, the nine-member arm of the IDPH that holds public hearings for new applications for in-state medical buildings and passes its recommendations to the main IDPH office in Springfield, said that a lengthy public hearing for the proposal is “very likely, as the project is affiliated with the University of Chicago.”
Avery declined to clarify her statement, but sent the Weekly a fifty-page transcript of the proceedings of the last time that the IDPH received a UCMC proposal, in August 2014. The plan, which was approved, was to build a $66.9 million medical office building in Orland Park, which is due to be completed in 2018. In the minutes for the public hearing, Sharon O’Keefe, the CEO of UCMC, discussed UCMC’s role in South Side trauma care at length when prompted by Board Vice Chairman John Hayes. She emphasized the UCMC’s focus on pediatric trauma care, even though the subject was not directly relevant to the proposal.
However, UCMC representatives declined to comment altogether about the planned facility at Holy Cross.
But in the shadow of the trauma center announcement, one contingent has been almost completely silent on the subject: the activist groups that petitioned and protested the UCMC for years to build an Adult Level I Trauma Center at its Hyde Park facility. Students for Health Equity (SHE), Fearless Leading by the Youth (FLY), and Southside Together Organizing for Power (STOP), under the banner of the Trauma Care Coalition (TCC), routinely brushed with the Chicago Police Department in efforts to make their demands heard; at a protest in June, nine participants were arrested. In a statement dated September 10, the same day that UCMC and Sinai announced the plan to build a trauma center at Holy Cross, the TCC released a statement that argued that the location of Holy Cross still leaves “large swaths of the South Side that will not be adequately served by the new trauma center,” as the boundaries of some South Side neighborhoods, such as South Shore, are more than five miles away from the hospital.
While representatives for FLY and STOP declined to comment for this story, Anna Nathanson, a UofC student and member of SHE, said that the activists’ relative quiet is not a reflection of apathy, but rather is about taking time to assess a proposal that is really a public relations gambit. She added that the University’s plan to co-operate an Adult Level I Trauma Center at a facility other than the UCMC is consistent with its goal of “keeping young black people away from their campus.”
“Some of this gets into theories of why social dislocation works. It’s embarrassing for [UofC] alumni to hear about their alma mater’s moral failures, so the proposal at Holy Cross is to make the appearance that the university is doing the right thing,” Nathanson said. She added that she disagrees that most potential trauma patients would be insured, including under Medicaid managed care.
“This stays in line with the UCMC’s policy of keeping the hospital as profitable as possible,” she said.
Nathanson said that SHE is currently soliciting “input” from residents who live near Holy Cross Hospital. She declined to comment on what questions SHE is asking Chicago Lawn residents in order to compile this input.
While Merlotti said that he has not spoken with SHE, STOP, or FLY since the UCMC announced the Holy Cross proposal, he credited activist groups with convincing the University to follow through with the project.
“I cannot say what they’re thinking now, outside of what I’ve read in the papers,” he said. “They just maintained a public awareness of the issue, and they made the University of Chicago believe that they did want to collaborate with us. I think community activism played a role in the University saying yes.”